Zooming in on Cutaneous Leishmaniasis: The Hidden Scars of a Neglected Disease
Image: Leishmania mexicana parasites in the promastigote stage, SEM. University of Oxford, Richard Wheeler. Source: Wellcome Collection.
Select Reading Level
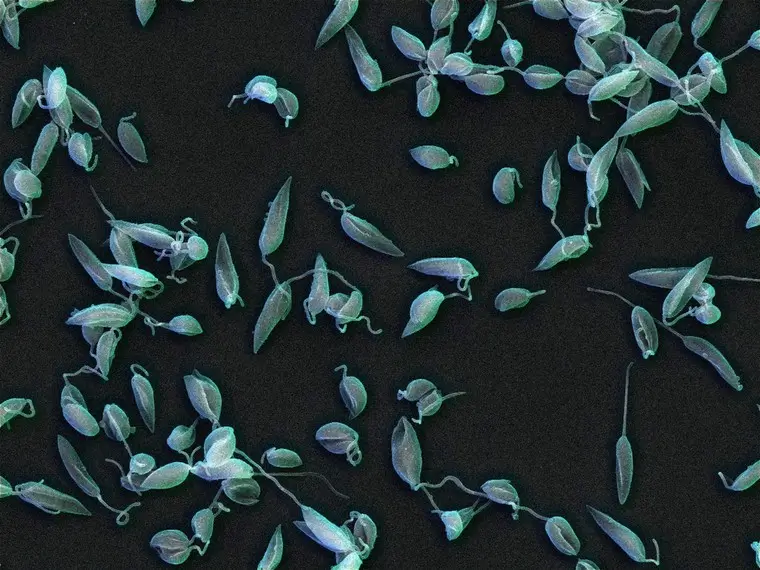
Image: Leishmania mexicana parasites in the promastigote stage, SEM. University of Oxford, Richard Wheeler. Source: Wellcome Collection.